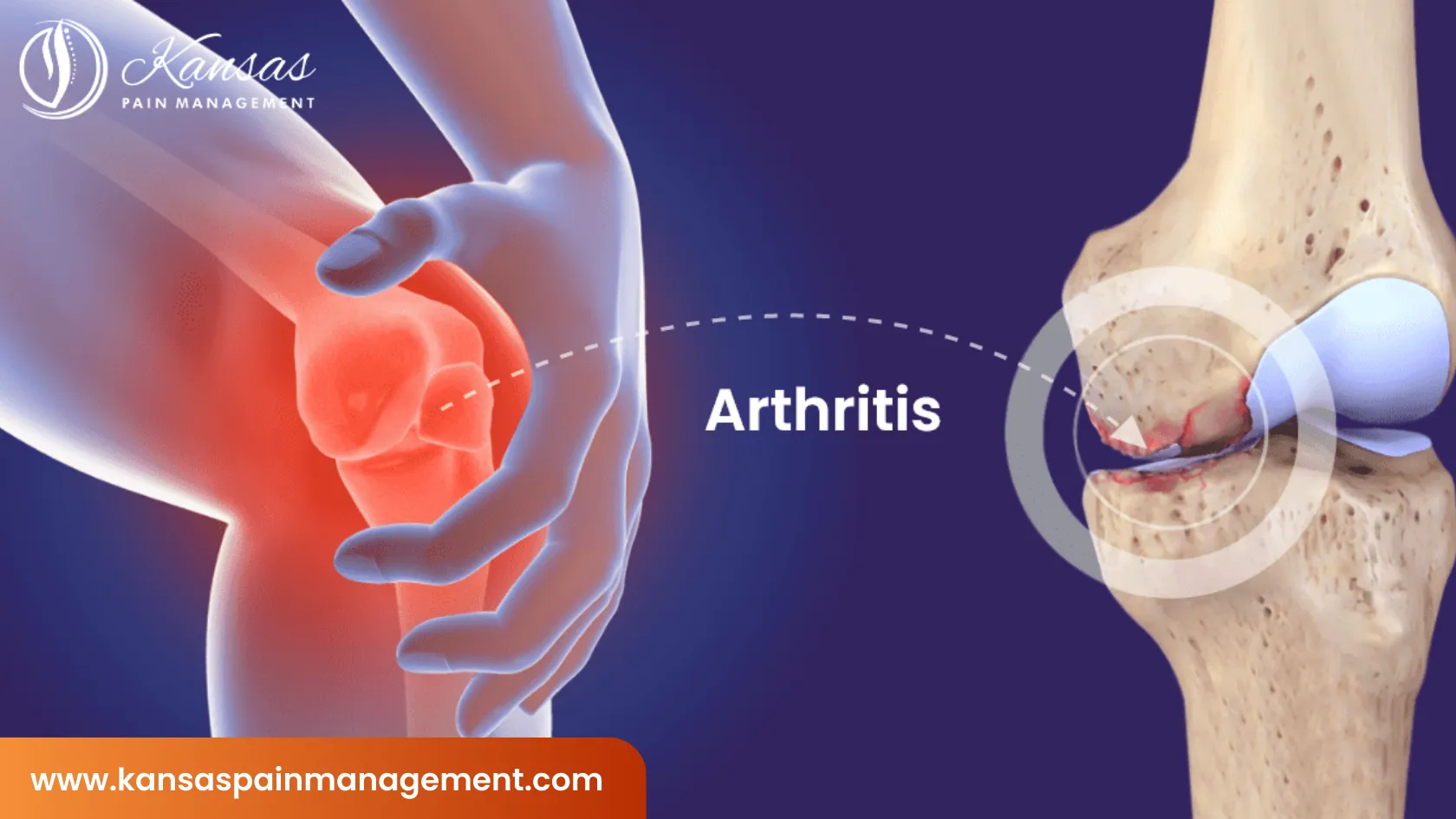
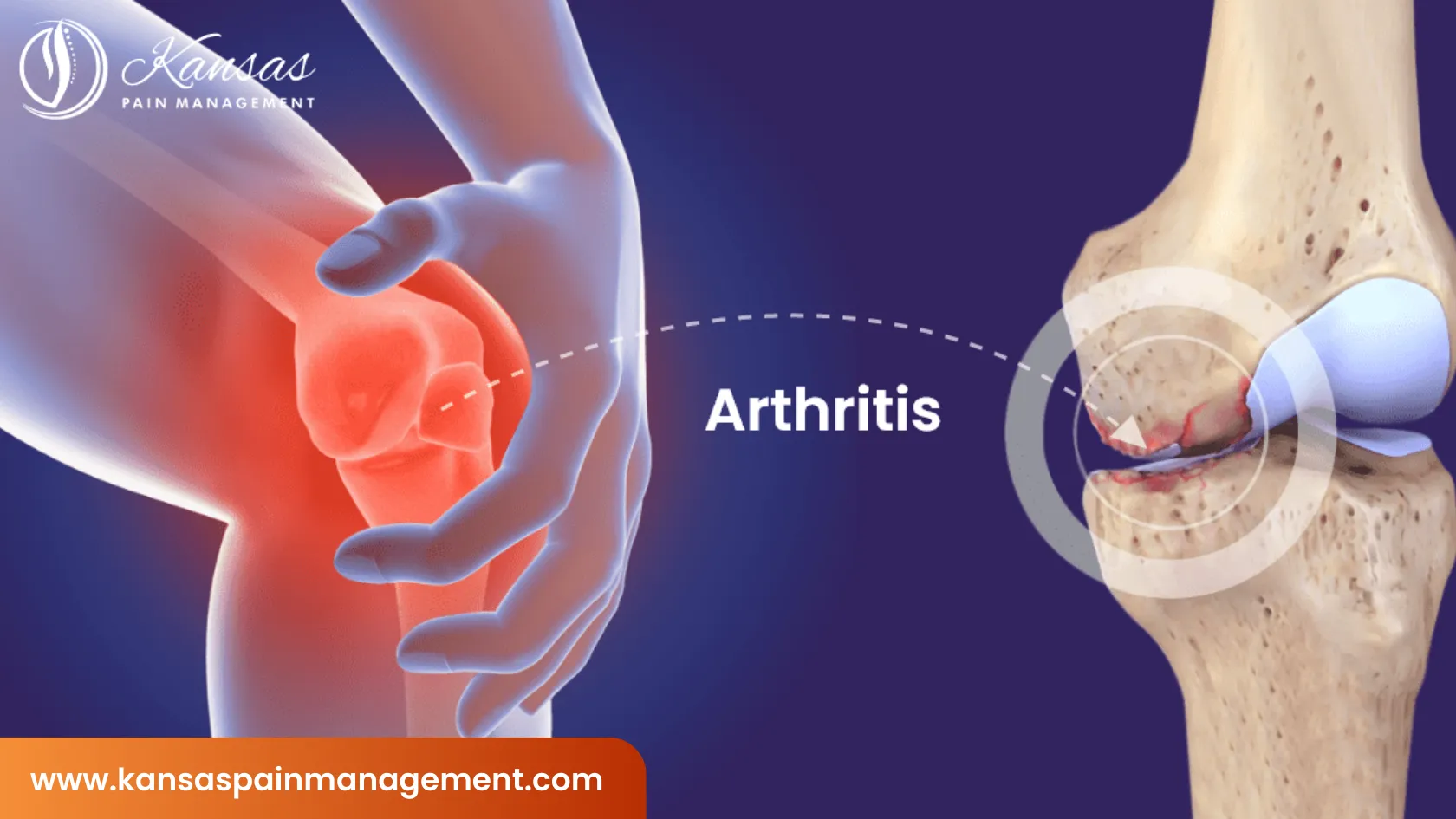
Understanding Arthritis: A Comprehensive Guide to Managing Joint Health
Arthritis is not a single disease; it is an informal way of referring to more than 100 types of joint diseases and related conditions. People of all ages, sexes, and races can and do have arthritis, and it is the leading cause of disability in many countries. Common symptoms include swelling, pain, stiffness, and decreased range of motion. These symptoms can come and go, and they can be mild, moderate, or severe.
While some forms of arthritis stay about the same for years, others may progress and get worse over time. Severe arthritis can result in chronic pain, inability to do daily activities, and make it difficult to walk or climb stairs. Arthritis can cause permanent joint changes, which may be visible, such as knobby finger joints, but often the damage can only be seen on an X-ray. Some types of arthritis also affect the heart, eyes, lungs, kidneys, and skin as well as the joints.
1. The Early Signs and Initial Symptoms
The onset of arthritis is often subtle, beginning with a slight stiffness in the morning that seems to dissipate as you move throughout the day. You might notice a nagging ache in a specific joint after a period of activity, or perhaps a localized swelling that doesn't seem to have a clear cause. These early signals are the body’s way of communicating that the cartilage—the slick, cushioning surface on the ends of bones—may be wearing thin or that the immune system is misfiring.
As the condition progresses, the frequency of these "flares" may increase. You might find that tasks requiring fine motor skills, such as buttoning a shirt or turning a key, become increasingly frustrating. It is during this early stage that many people dismiss their discomfort as "just getting older," yet this is the most critical time for early intervention and diagnosis to prevent long-term structural damage.
2. Understanding the Core Types: Osteoarthritis vs. Rheumatoid Arthritis
To manage the condition, one must understand the difference between the two most common types. Osteoarthritis (OA) is the most prevalent form, often called "wear and tear" arthritis. It occurs when the protective connective tissue breaks down over time. In contrast, Rheumatoid Arthritis (RA) is an autoimmune disorder where the immune system attacks the synovium—the lining of the membranes that surround your joints.
While OA is typically localized to specific joints like the knees, hips, or hands, RA is a systemic disease that can affect the entire body. RA often presents symmetrically, meaning if one wrist is inflamed, the other likely is too. Understanding these distinctions is vital because the treatment protocols for a mechanical breakdown are vastly different from those required to suppress an overactive immune response.
Key Differences at a Glance
- Osteoarthritis: Focuses on cartilage breakdown; usually starts later in life; morning stiffness lasts less than 30 minutes.
- Rheumatoid Arthritis: Focuses on the synovial membrane; can start at any age; morning stiffness lasts longer than an hour.
3. The Pathophysiology: What Happens Inside the Joint
At the molecular level, arthritis involves a complex cascade of inflammatory mediators. In a healthy joint, the synovial fluid acts as a lubricant, allowing for frictionless movement. When arthritis strikes, this balance is disrupted. In inflammatory types, the body releases cytokines, such as TNF-alpha and interleukins, which trigger a cycle of swelling and tissue destruction that eventually erodes the bone itself.
In degenerative cases, the loss of proteoglycans within the cartilage matrix causes the tissue to become brittle and thin. As the cartilage disappears, bone rubs on bone, leading to the development of osteophytes (bone spurs). These spurs can limit movement and cause significant pain as they press against nerves or neighboring tissues. The structural integrity of the ligaments and tendons surrounding the joint may also weaken, leading to joint instability.
4. Risk Factors and Preventative Measures
While genetics play a significant role in your likelihood of developing arthritis, several environmental factors are within your control. Obesity is a primary risk factor, especially for weight-bearing joints like the knees and hips. Excess weight doesn't just add mechanical stress; fat tissue produces proteins that can cause inflammation in and around your joints.
Preventative measures focus on joint protection and lifestyle choices. Maintaining a healthy weight, avoiding repetitive occupational injuries, and staying active can significantly lower your risk. It’s also essential to manage blood sugar levels, as high glucose can stiffen the fibers that support your cartilage and make joints more susceptible to compression.
Strategies for Prevention:
- Low-impact exercise: Swimming or cycling to maintain muscle strength without taxing the joints.
- Proper ergonomics: Using supportive chairs and tools at work to reduce joint strain.
- Nutrition: Consuming a diet rich in antioxidants and Omega-3 fatty acids.
5. Diagnostic Procedures and Medical Imaging
When you visit a specialist, typically a rheumatologist, the diagnostic process begins with a physical exam and a detailed medical history. The doctor will check for redness, warmth, and range of motion. However, to see what is happening beneath the skin, physicians rely on diagnostic imaging. An X-ray can show bone erosion and joint space narrowing, while an MRI provides a more detailed look at the soft tissues like cartilage and tendons.
In addition to imaging, laboratory tests are crucial for identifying inflammatory markers. Blood tests may look for the Rheumatoid Factor (RF) or Anti-CCP antibodies. They might also check the Erythrocyte Sedimentation Rate (ESR) or C-Reactive Protein (CRP) levels, which indicate the level of general inflammation in the body. In some cases, a doctor may perform an arthrocentesis—withdrawing a sample of joint fluid for analysis.
6. Modern Treatment Modalities: Medications
The pharmaceutical approach to arthritis has evolved tremendously. For basic pain management, Nonsteroidal Anti-inflammatory Drugs (NSAIDs) like ibuprofen are commonly used to reduce both pain and inflammation. However, for chronic autoimmune conditions, doctors often prescribe Disease-Modifying Antirheumatic Drugs (DMARDs), which work to slow the progression of the disease rather than just masking the symptoms.
A more recent breakthrough involves biologic response modifiers. These are genetically engineered proteins that target specific parts of the immune system that fuel inflammation. While highly effective, these medications require careful monitoring by a healthcare provider due to potential side effects, including an increased risk of infections. For localized relief, corticosteroid injections can be administered directly into the joint to provide rapid, temporary relief from severe swelling.
7. The Role of Physical and Occupational Therapy
Medicine is only one piece of the puzzle; rehabilitation is equally vital. A physical therapist can design a customized exercise program to strengthen the muscles surrounding the joint, which acts as a natural "brace." They focus on flexibility and balance, which are essential for preventing falls and maintaining independence. Using heat and cold therapies can also help manage the vasodilation and vasoconstriction needed to control pain and stiffness.
Occupational therapy (OT) focuses on "joint protection" during daily activities. An OT might suggest using assistive devices, such as jar openers, long-handled shoehorns, or specialized grips for pens. These modifications reduce the mechanical stress on small joints in the hands and wrists, allowing patients to perform their "occupations" or daily tasks with less discomfort and greater efficiency.
8. Nutritional and Lifestyle Adjustments
Dietary choices can influence the level of systemic inflammation in the body. The "Mediterranean Diet," rich in olive oil, fish, whole grains, and colorful vegetables, has been shown to have anti-inflammatory properties. Conversely, diets high in processed sugars and trans fats can exacerbate arthritic flares. Maintaining a focus on micronutrients like Vitamin D and Calcium is also important for supporting the underlying bone structure.
Beyond diet, sleep hygiene and stress management are critical. Chronic pain often leads to poor sleep, which in turn lowers the pain threshold, creating a vicious cycle. Techniques such as mindfulness-based stress reduction (MBSR) and yoga can help patients cope with the psychological burden of a chronic illness. Hydration is also key, as the cartilage is largely composed of water and requires fluid to remain supple and shock-absorbent.
9. Surgical Interventions: When Conservative Care Fails
When non-invasive treatments no longer provide adequate relief, surgical options may be considered. One of the most common procedures is arthroscopy, where a surgeon uses a small camera and instruments to repair soft tissue tears or "clean out" debris within the joint. For those with severe joint destruction, a total joint replacement (arthroplasty) may be necessary, where the damaged joint is replaced with a prosthetic made of metal, plastic, or ceramic.
Another option for smaller joints, like those in the fingers or ankles, is joint fusion (arthrodesis). This procedure removes the damaged surfaces and fuses the bones together until they heal into one solid unit. While this eliminates movement in that specific joint, it is highly effective at eliminating unbearable pain. Recovery from these surgeries requires intensive post-operative physical therapy to regain strength and function.
10. Living with Arthritis: Long-term Outlook
Living with arthritis requires a shift in perspective—moving from seeking a "cure" to mastering disease management. Because it is often a lifelong journey, building a strong support network of family, friends, and medical professionals is essential. Staying informed about the latest clinical trials and research can also provide hope and access to new therapies that may improve your quality of life.
The long-term goal is to maintain mobility and prevent disability. By combining medical treatments with lifestyle modifications and a positive mental attitude, most people with arthritis can continue to lead active, fulfilling lives. It is about listening to your body, knowing when to rest, and knowing when to push through, all while working closely with your rheumatology team to adjust your plan as your needs change over time.
Conclusion
In summary, arthritis is a multifaceted condition that requires a proactive and holistic approach to management. From the early recognition of joint stiffness to the advanced stages requiring potential surgical intervention, the key is consistency and education. By understanding the pathophysiology of your specific type of arthritis and implementing a combination of medical, physical, and nutritional strategies, you can take control of your health. Remember, while the bones and joints may be the focus, treating the "whole person" is what leads to the best outcomes.